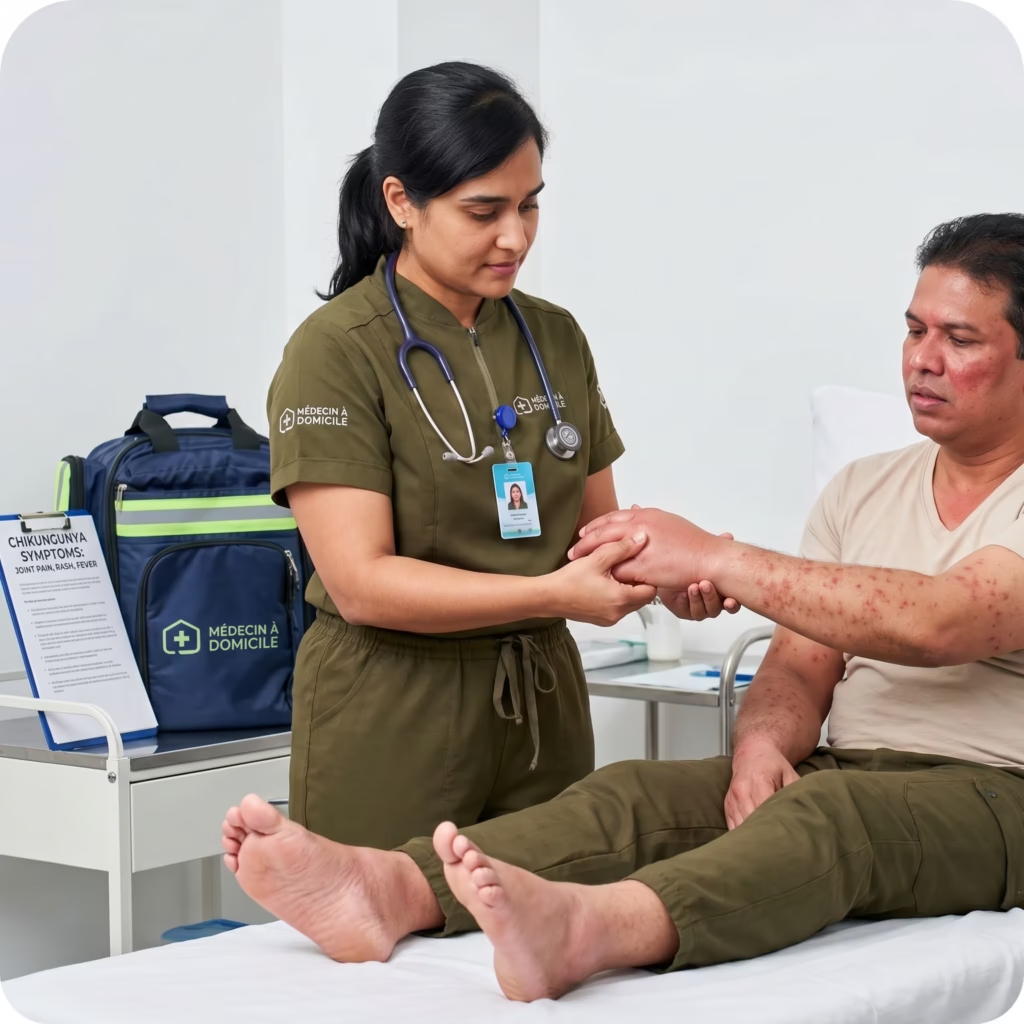
Chikungunya in Mauritius: Symptoms, Treatment, and How to Protect Your Family
Chikungunya is a mosquito-borne viral infection that has re-emerged as a significant health concern in Mauritius and the wider Indian Ocean region. In 2025, Mauritius recorded the highest number of chikungunya cases in the African region according to the WHO, following confirmed cases in Pereybere, Plaine Magnien, and other areas across the island. The neighbouring island of Reunion experienced a major outbreak in the same period, with an estimated 66% seroprevalence in the population.
The virus causes sudden fever followed by severe, debilitating joint pain that can last weeks, months, or in some cases years. While rarely fatal, chikungunya can significantly affect quality of life and daily functioning, particularly in elderly patients and those with pre-existing joint conditions.
This guide covers everything families in Mauritius need to know: what chikungunya is, how to recognise it, how it differs from dengue, how to manage symptoms at home, and when medical attention is needed.
What Is Chikungunya?
Chikungunya is a viral infection transmitted to humans through the bite of infected Aedes mosquitoes, the same type of mosquito that spreads dengue fever. In Mauritius, the primary vector is Aedes albopictus, which bites mainly during daytime hours, particularly in the early morning and late afternoon.
The name “chikungunya” comes from a word in the Kimakonde language meaning “to become contorted” or “that which bends up,” referring to the stooped posture caused by the intense joint pain the virus produces.
Mauritius experienced its first major chikungunya outbreak in 2005-2006. After years of relative quiet, the virus returned in 2025 with locally acquired cases confirmed across the island, raising concerns about a potential resurgence during the 2025-2026 mosquito season.
There is currently no specific antiviral treatment for chikungunya. Management focuses on relieving symptoms, particularly the joint pain, and supporting recovery.
Recognising Chikungunya Symptoms
Symptoms typically appear 4 to 8 days after being bitten by an infected mosquito, though the incubation period can range from 2 to 12 days. Not everyone who is infected will develop symptoms, but those who do usually experience a distinctive pattern.
Acute phase (first 1-2 weeks)
- Sudden high fever (often 39-40 degrees C), usually lasting 2 to 7 days
- Severe joint pain, typically affecting the hands, wrists, ankles, feet, and knees. The pain is often symmetrical (both sides of the body)
- Joint swelling and stiffness
- Muscle pain throughout the body
- Headache
- Skin rash, usually appearing 2 to 5 days after fever onset, often on the trunk and limbs
- Fatigue and general weakness
- Nausea
What makes chikungunya different from other fevers
The hallmark of chikungunya is the severity of the joint pain. While dengue also causes body aches, chikungunya joint pain is typically more intense, more localised to the joints (not just general muscle aches), and can be so severe that patients struggle to walk, grip objects, or perform basic daily activities. This is the distinguishing feature that sets it apart from dengue and other febrile illnesses.
Chronic joint pain (post-acute phase)
This is the most challenging aspect of chikungunya. In many patients, the joint pain persists long after the fever resolves. Studies show that 30 to 60% of patients continue to experience joint pain for weeks to months, and some for over a year. Elderly patients, those with pre-existing arthritis, and those who experienced severe acute symptoms are at higher risk of chronic joint involvement.
Persistent symptoms can include morning stiffness, joint pain that fluctuates in intensity, swelling that comes and goes, fatigue, and difficulty with fine motor tasks like writing or buttoning clothes.
Chikungunya vs Dengue: How to Tell the Difference
Since both chikungunya and dengue fever are spread by the same mosquito and circulate in Mauritius during the same seasons, distinguishing between them is important for proper management.
The key differences are that joint pain is the dominant symptom in chikungunya while dengue tends to cause more generalised body and muscle pain, that chikungunya joint pain is typically symmetrical (both wrists, both ankles) while dengue pain is more diffuse, that dengue is more likely to cause pain behind the eyes, that bleeding complications are associated with severe dengue but not chikungunya, and that chronic joint pain lasting months is a feature of chikungunya but not dengue.
However, the two infections can look very similar in the first few days. A doctor can clinically distinguish between them and arrange blood tests for confirmation if needed. It is also possible, though uncommon, to be infected with both viruses simultaneously.
Managing Chikungunya at Home
Since there is no antiviral cure, treatment focuses on managing symptoms and supporting the body’s recovery.
For the acute phase (fever and early joint pain)
- Rest is essential. The body needs energy to fight the virus
- Stay hydrated with water, oral rehydration solutions, coconut water, and clear soups. Fever increases fluid loss
- Take paracetamol for fever and pain. Follow recommended dosages
- Avoid aspirin and ibuprofen until dengue has been ruled out, as these can increase bleeding risk in dengue. Once a doctor confirms chikungunya (not dengue), anti-inflammatory medications like ibuprofen may be appropriate for joint pain
- Apply cold compresses to swollen, painful joints for 15 to 20 minutes at a time
- Gentle movement of affected joints can help prevent stiffness, but avoid strenuous activity
For persistent joint pain (post-acute phase)
If joint pain continues after the fever has resolved, ongoing management may include anti-inflammatory medication prescribed by a doctor, gentle physiotherapy exercises to maintain range of motion, adequate rest balanced with light activity to prevent deconditioning, and regular medical follow-up to monitor progress and adjust treatment.
Chronic chikungunya joint pain can be frustrating and demoralising. If pain persists beyond 2 to 3 weeks after the fever resolves, a medical review is recommended to discuss ongoing management options.
How to Prevent Chikungunya in Mauritius
Prevention is identical to dengue prevention because the same mosquito species transmits both viruses. Protecting yourself from Aedes mosquito bites is the only way to prevent infection.
Protect yourself from mosquito bites
- Use insect repellent containing DEET (20-30%) on exposed skin, especially during morning and late afternoon hours when Aedes mosquitoes are most active
- Wear long-sleeved shirts and long trousers when outdoors during peak mosquito activity
- Use mosquito nets over beds, particularly for infants, young children, and elderly patients
- Install or repair window and door screens
- Use electric mosquito repellent devices or coils indoors
Eliminate mosquito breeding sites
- Empty all containers that collect standing water: flower pot saucers, buckets, tyres, gutters, pet bowls
- Cover water storage tanks with tight-fitting lids
- Change water in vases and plant trays at least once a week
- Clear blocked drains and gutters regularly
- Dispose of old tyres, cans, and bottles that can collect rainwater
- Keep swimming pools chlorinated and maintained
These measures protect against both chikungunya and dengue simultaneously. A single uncovered container can produce hundreds of mosquitoes, so community-wide effort is essential.
When to Call a Doctor
While most chikungunya cases can be managed at home, certain situations require medical evaluation.
Call a doctor if:
- Fever persists beyond 5 days without improvement
- Joint pain is so severe that the patient cannot walk, use their hands, or perform daily tasks
- The patient cannot keep fluids down due to persistent nausea or vomiting
- Signs of dehydration appear: dry mouth, dark urine, dizziness
- The patient is an infant, a child under 5, or an elderly person
- The patient is pregnant
- The patient has a pre-existing condition (diabetes, heart disease, arthritis, immune suppression)
- Joint pain persists beyond 2 to 3 weeks after fever resolves
- You are unsure whether the illness is chikungunya, dengue, or another infection
A home doctor can assess the severity, distinguish chikungunya from dengue clinically, administer IV fluids for dehydration and pain medication, prescribe appropriate anti-inflammatory treatment once dengue is ruled out, and arrange blood tests for confirmation.
Medecin a Domicile provides 24/7 home doctor visits across Mauritius. Call 86121 at any time for a licensed doctor to visit your home.
Chikungunya in Elderly Patients
Elderly patients are at particular risk from chikungunya for several reasons. The severe joint pain can be disabling, especially for those who already have limited mobility. Pre-existing arthritis or joint conditions can be worsened by the infection. Dehydration from fever sets in faster in older patients. The chronic joint pain phase is more common and more severe in elderly patients.
For any elderly patient who develops sudden fever with joint pain during mosquito season, a home doctor assessment is strongly recommended. Treatment at home avoids the physical strain of hospital travel and the infection risk of waiting rooms. Learn more about elderly home doctor visits.
Chikungunya in Children
Children generally recover well from chikungunya, but the acute phase can be distressing. Young children may not be able to describe their symptoms clearly. Parents should watch for high fever, irritability or excessive crying, refusal to walk or use hands, skin rash, and reduced appetite or fluid intake.
If your child develops these symptoms during mosquito season, a pediatric home visit provides fast assessment in the environment where the child feels safest.
Frequently Asked Questions
Can you get chikungunya more than once?
Typically no. Once you have been infected with chikungunya, you develop lifelong immunity to the virus. Unlike dengue (which has 4 serotypes), there is only one chikungunya serotype, so reinfection is extremely rare.
Is there a vaccine for chikungunya?
A chikungunya vaccine has been developed and is available in some countries for certain populations. However, it is not yet widely available for general use in Mauritius. Prevention through mosquito bite avoidance remains the primary strategy.
How long does chikungunya joint pain last?
The acute joint pain typically improves within 1 to 3 weeks. However, 30 to 60% of patients experience some degree of joint pain for months after the initial infection, and a smaller percentage may have symptoms lasting over a year. Early medical management and appropriate anti-inflammatory treatment can help reduce the duration.
Can a doctor treat chikungunya at home?
Yes. A home doctor can assess the severity, prescribe medication for fever and joint pain, administer IV fluids for dehydration, distinguish chikungunya from dengue, and arrange follow-up care for persistent joint pain. Call 86121 for a home visit.
Is chikungunya dangerous?
Chikungunya is rarely fatal. The main concern is the severity and duration of joint pain, which can significantly affect quality of life. Elderly patients, newborns, and those with weakened immune systems are at higher risk of complications. Early medical assessment and proper symptom management make a significant difference in recovery.
Can chikungunya and dengue occur at the same time?
Yes. Since both are transmitted by the same mosquito species, co-infection is possible, though uncommon. A doctor can clinically evaluate the symptoms and arrange blood tests to confirm the diagnosis if needed.
Chikungunya is preventable through mosquito bite avoidance, and manageable with proper medical care. If you or a family member develops sudden fever with severe joint pain, do not wait. Call 86121 for a 24/7 home doctor visit anywhere in Mauritius. Visit medecin.mu for more information.